| 01923 | ||
| 255632 | ||
|
||||
| Send an email. |
Treatment of Fungal Nails (Onychomycosis)
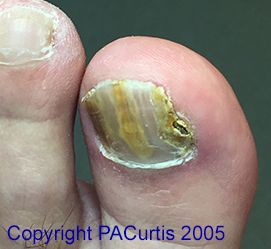
Onychomycosis is usually caused by one or more of several possible fungal organisms managing to penetrate beneath the free edge of the nail plate and starting to grow. Over time they gradually move closer to the bottom of the nail, eventually disappearing beneath the cuticle (eponychium). Initially there is usually an element of trauma involved, which separates the nail plate from the underlying nail-bed, thus allowing ingress of the fungal spores.
Very often there will also be a chronic skin infection of the whole foot by the same fungal organism that causes the nail problem; this will usually predate the nail infection. This chronic infection does not present in the same way as an acute attack of "Athlete's Foot", with which most people will be familiar, where the area is red, inflamed, itchy and possibly moist. Rather, it causes a dryness of the whole foot, usually in a "slipper" pattern. It needs to be addressed at the same time that the nail is treated in order to reduce the risk of reinfection.
On occasion the nail infection may be caused by a mould (e.g. Scopulariopsis brevicaulis or members of the Neoscytalidium or Aspergillus families) which grows on the upper surface of the nail, rather like the mould that covers cheeses such as brie and camembert. Another culprit may be a yeast, such as Candida albicans, which is also responsible for thrush. The greatest number of infections, however, are caused by a group of fungi called dermatophytes and the commonest of these is Trichophyton rubrum.
Fungal infections of the skin and nails of the feet can be spread to the top of the inner thighs as one dresses, causing an unpleasant infection. It is more common in men than women and goes by such names as "Dhobi itch" and "Jock itch".
Surgeons may be reluctant to carry out procedures on people with either chronic or acute fungal infections because of the risk of contaminating wounds, particularly if there is to be an implant, such as a new hip or knee joint.
Apart from removing the whole nail and preventing it from ever regrowing, there is no single treatment that is guaranteed to work every time on every patient. This makes treating the condition frustrating, both for the practitioner and the patient.
Treatments available include:
ORAL: A course of tablets such as terbinafine, itraconazole or griseofulvin may be taken for between three and six months. This is effective in, perhaps, 70% of cases but may cause a range of side effects ranging from rashes and upset stomachs, through joint and muscle pain to serious liver dysfunction. Liver function tests will be required, both before and during a course of treatment.
There is good evidence to suggest that the efficacy of oral treatment is greatly enhanced if a topical agent is used concurrently.
FENESTRATION: This involves painlessly creating a series of tiny holes in the nail plate, thus allowing an antifungal agent to penetrate through to where the infection lies. While the medicament used is very similar to that used in the oral treatment the risk of undesirable side effects is virtually eliminated since it is only used locally. There is, of course, the small chance of allergy or local irritation, but this is most unusual.
Fenestration is the treatment that we most favour at Nascot Podiatry, where we use the Clearanail system. This involves a very clever, specially designed, micro-cutter tool creating tiny holes in the nail plate - the clever bit being that the process stops before it reaches the sensitive tissue of the nail bed. Both research and personal experience show success rates very similar to oral treatment - but without the associated health risks.
TOPICAL: There are a number of preparations available which are applied to the surface of the nail, either daily or weekly. They can be effective if the infection has only spread a little way down the nail but are often compromised by poor patient compliance - it can be a bit of a trial to carefully apply the lacquer for the requisite period of time, which may be a year or more. At the end of the day the success rate for this type of treatment is, generally, significantly less than fifty percent.
Some folk will, occasionally, advocate the application of such things as tea-tree oil, aloe vera or Vick's vapour rub. These treatments appear to have little merit and tend to be consigned to the "eye of newt" school of medicine.
LASER: Several companies offer "cold laser" devices for the treatment of fungal nails. The equipment is expensive, meaning that the treatment episodes tend to be equally expensive. There are also conflicting schools of thought as to the efficacy of such treatments, particularly in the long-term.
Links To Other Websites:
Copyright © P.A.Curtis, 2026.


